Understanding Late-Onset Autoimmunity

While autoimmune disease is often associated with young or middle-aged adults, it can emerge for the first time later in life. Evidence suggests that diagnoses among older adults are increasing, raising new questions about how immune aging, hormonal changes, and environmental exposures shape disease risk.
To better understand why autoimmunity appears in later decades, Frederick Miller, MD, PhD, former head of the Environmental Autoimmunity Group at the National Institute of Environmental Health Sciences, and Andrea George, MD, an endocrinologist at Hill Country Endocrinology in Austin, Texas, share their perspectives on the factors driving this growing trend.
Why Are More Autoimmune Diseases Being Diagnosed Later in Life?
“It is a complex interplay of differences in exposures, hormones, and epigenetic effects that build up over decades and impact different immune compartments.”
– Frederick Miller, MD, PhD
Research studies reveal a rise in certain autoimmune diseases (1). A study in the journal Arthritis & Rheumatology highlights this trend, finding that anti-nuclear antibodies (ANA) increased in certain groups of people between 1988 and 2012 (2). The presence of ANA can be a sign of an autoimmune disease such as systemic lupus erythematosus, scleroderma, and Sjögren’s syndrome.
The study also found that people over 50 were among the groups with the most significant increase in ANA.
Our rapidly changing environment increasingly strains our immune systems, requiring constant adaptation. These changes, in addition to some lifestyle changes, may have a cumulative effect over time.
Specific factors have been linked to the rise of autoimmune diseases, and older people might be particularly vulnerable to them (3) :
- Diet: Poor-quality diets high in processed foods and additives may be harmful.
- Environmental toxins: Exposure to potentially harmful chemicals in household products is increasing.
- Air pollution: Vehicle and factory exhaust reduce air quality.
- Infections: Some infections can trigger autoimmune responses.
- Lifestyle challenges: Sleep deprivation and chronic stress can negatively impact health.
- Climate change: Climate shifts may be linked to new pathogens and food-borne illnesses.
Dr. George also noted an even greater increase in certain autoimmune diseases since the beginning of the COVID-19 pandemic.
“Post COVID, we have seen a significant increase of autoimmune disease, including latent autoimmune diabetes in adults in patients with no prior history or family history of autoimmune disease.”
– Andrea George, MD
Why Does Autoimmunity Increase With Age?
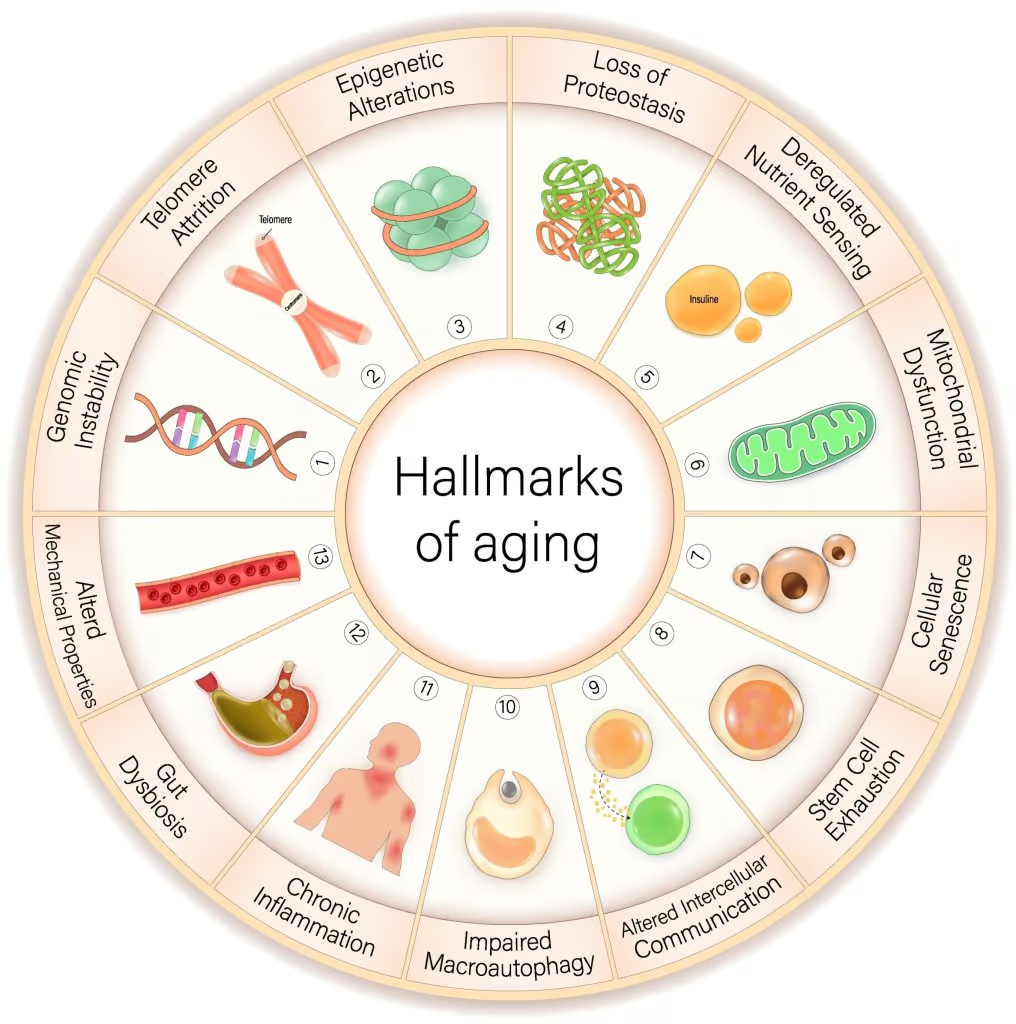
As we age, our immune system undergoes age-related changes, immunosenescence, leading to increased autoimmunity (4). Our bodies begin to make more autoantibodies that can lead to autoimmune diseases. At the same time, our aging immune systems weaken, making us less able to fight off disease.
A weakened immune system combined with increased autoimmune triggers makes older people a unique target for the development of late-onset autoimmune disease.
How Do Autoimmune Symptoms Present in Older Adults?
Older people can present with vague or atypical symptoms of autoimmune diseases. For example, older people with SLE might present with weight loss, muscle pain, and cognitive, behavioral, or mood deterioration (5).
Dr. Miller cautions, “Some believe that older people do not develop new autoimmune diseases, so they are sometimes not adequately screened or assessed for these when they develop new syndromes. Also, since late-onset autoimmune diseases can present atypically, they can be misdiagnosed more frequently as other conditions.”
Healthcare providers should consider late-onset autoimmune disease when older people present with new or unusual complaints. With respect to latent autoimmune diabetes in adults (LADA), Dr. George says, “The main challenges are due to the lack of awareness and education on accurately diagnosing LADA. It has always been taught, even in medical school, that a patient with diabetes diagnosed at a young age is consistent with autoimmune diabetes (Type 1) and a patient diagnosed at an older age most likely has Type 2″.
Why Are Women at Higher Risk for Autoimmune Disease?
Women are disproportionately affected by autoimmune diseases, with factors such as genetics, hormonal changes, and social/environmental influences contributing to this disparity. A recent review suggests that social (such as environmental exposures, access to healthcare, and dietary) and cultural factors (gender differences) are also possible culprits (6).
Women are at particular risk for developing an autoimmune disease at times of increased stress, such as pregnancy, or during a significant hormonal change (7). In addition to other age-related factors, menopause related hormonal changes might be an additional risk factor for late-onset autoimmune diseases.
Can You Develop More Than One Autoimmune Disease?
People with one autoimmune disease are more likely to develop other autoimmune diseases. When someone has three or more autoimmune diseases, it is called multiple autoimmune syndrome (MAS).
According to Dr. Miller, “Given the shared genetic and environmental risk factors for many autoimmune diseases, it is common for people with one autoimmune disorder to develop others, and this increases over time as more environmental exposures and infections accumulate.” Older adults, who’ve likely had more environmental exposures and are more susceptible to infection, might be at risk for developing MAS.
Certain autoimmune diseases are more likely than others to present with another autoimmune disease. For example, systemic lupus erythematosus may coexist with Sjögren’s syndrome (8) and rheumatoid arthritis with autoimmune thyroiditis.
Managing Late-Onset Autoimmune Disease
Although late-onset autoimmune diseases can be challenging to spot, they can be well-managed once diagnosed. Additionally, symptoms are generally milder than those seen in younger people (9).
Living with an autoimmune disease can significantly impact quality of life. They can also bring considerable costs to the healthcare system across the lifespan. Early diagnosis and treatment can help slow progression and minimize these diseases’ impact on your life. If you are experiencing symptoms that you can’t explain, see a healthcare provider for help.
What’s Next for Late-Onset Autoimmune Disease Research?
More research on late-onset autoimmune diseases is needed. Currently, most research focuses on younger adults. Dr. Miller notes, “There is a lack of systematic databases and registries for autoimmune diseases to understand how late-onset autoimmune disease presents and its natural history.” He points to “the general lack of mechanistic and therapeutic studies of late-onset autoimmune disease.”
Treatment approaches for younger adults can guide diagnosis and treatment until more research is available. As research grows, so will our understanding of the treatment options for these diseases.

About the Author
Sources
- Article Sources
Conrad N. et al. (2023). Incidence, prevalence, and co-occurrence of autoimmune disorders over time and by age, sex, and socioeconomic status: a population-based cohort study of 22 million individuals in the UK. Lancet, 401(10391), 1878–1890.
Dinse G. E. et al. (2020). Increasing Prevalence of Antinuclear Antibodies in the United States. Arthritis & Rheumatology, 72(6), 1026–1035.
Miller F. W. (2023). The increasing prevalence of autoimmunity and autoimmune diseases: An urgent call to action for improved understanding, diagnosis, treatment, and prevention. Current Opinion in Immunology, 80, 102266.
Kurup S. et al. (2024) Biochemistry, Autoimmunity. StatPearls.
Azar A. et al. (2023). Immune function in older adults. UpToDate.
Calabrò A. et al. (2023). Sex and gender affect immune aging. Frontiers in Aging, 4, 1272118.
Angum F. et al. (2020). The Prevalence of Autoimmune Disorders in Women: A Narrative Review. Cureus, 12(5), e8094.
Pasoto S. G. et al. (2019). Sjögren’s syndrome and systemic lupus erythematosus: links and risks. Open access Rheumatology: research and reviews, 11, 33–45.
Watad A. et al. (2017). Autoimmunity in the Elderly: Insights from Basic Science and Clinics – A Mini-Review. Gerontology, 63(6), 515–523.