Autoimmune vs Autoinflammatory Disease
A Comparative Look
Countless scientific studies have been conducted in the name of immunology, the study of human immunity. Scientists look to the immune system for a better understanding of asthma, allergies, cancer, metabolic diseases, and many other health conditions. Likewise, researchers are seeking to understand how and why the immune system malfunctions in some individuals. Abnormal activation of the immune system can point to many different diseases that cause chronic inflammation, tissue destruction, and more. Autoimmune disease (AD) and autoinflammatory disease (AIF) are two categories of illnesses that occur when the immune system mistakenly damages healthy cells. Although these inflammatory disorders share many commonalities, there are key features that make them unique.
The immune system is where it all begins
In order to describe the differences between autoimmune disease and autoinflammatory disease, it’s necessary to understand a few key facts about immunological function. The human immune system is a complex network of components that work to neutralize infections and protect the body from disease. Within the immune system are two lines of defense: innate immunity and adaptive immunity (1). The innate immune system includes defensive barriers such as the skin and mucous membranes, as well as an army of chemicals and cells that target disease-causing pathogens (2,3).
When provoked, the innate immune system releases an onslaught of these defensive properties. Some innate cells also secrete cytokines, which are proteins that deliver signals between immune cells. Additionally, cytokines play an important role in regulating fever and inflammation during an immune response (4). Innate immunity can mobilize quickly, usually within minutes to hours of encountering a threat. Activity from an innate immune response summons the body’s second line of protection, known as the adaptive immune system (5).
When provoked, the innate immune system releases an onslaught of these defensive properties.
Both innate and adaptive immunity can be activated by antigens, which are molecular structures that exist on the surface of human and pathogen cells (6). However, innate immunity can only identify the presence of foriegn antigens. Adaptive immunity recognizes specific foreign antigens and also builds specialized defenses against them. T cells and B cells are key players in the adaptive immune response (7). Together, these cells “memorize” the antigens of infectious agents, allowing the immune system to build a swift and targeted defense against repeat infections (8). Adaptive immune cells are hard-wired to ignore host cell antigens. Known as self-tolerance, this mechanism prevents the immune system from attacking healthy human tissues (9).
What is an autoinflammatory disease (AIF)?
Most distinctly, autoinflammatory diseases only involve the innate immune system. AIFs occur when innate immune cells are activated without an infection or injury being present. This mishap kickstarts the release of cytokines and other immune responses, causing fever and inflammation. Recurring episodes of high fever are the primary symptom of AIF (10). Similar to some autoimmune diseases, autoinflammatory symptoms can be widespread, affecting the joints, gastrointestinal tract, skin, eyes, and internal organs.
Autoinflammatory diseases are caused by mutations in the genes that control and regulate innate immune cells (11). Some AIFs, including Familial Mediterranean Fever (FMF) and TNF receptor–associated periodic syndrome (TRAPS), are known as monogenic because they are caused by a singular known genetic defect (12,13). Because these diseases originate in the genes, they can run in families (10).
Autoinflammatory syndromes are very rare. Presently, there is no known gender prevalence (14). Unlike autoimmune disease, the majority of AIFs develop during childhood. Due to the rarity of these diseases and their close appearance to other illnesses, diagnosis is often delayed (15). Several AIFs are known for their higher frequencies within certain ethnicities. As such, age of onset and familial history, in addition to clinical observations, can be helpful in diagnosing these rare conditions. In some cases, testing for gene mutations is used to confirm a diagnosis of AIF (12,16,).
What is an autoimmune disease (AD)?
While problems with innate immunity cause autoinflammatory diseases, autoimmune disease originates in the adaptive immune system. AD occurs when adaptive immune cells lose their ability to maintain self-tolerance of human cells. As a result, the immune system begins attacking healthy tissues as though they were infectious agents. Some ADs are organ-specific, whereas others can affect multiple parts of the body. Like autoinflammatory syndromes, recurrent fever, and chronic inflammation can be attributed to autoimmune disease. However, many possible symptoms are unique to AD, including hair loss, dry mouth, temperature sensitivity, muscle weakness, reproductive issues, and more.
Researchers believe that a variety of conditions including environment, hormones, injury, infection, and genes could all play a role in initiating autoimmunity.
AD is thought to be triggered by a combination of multiple factors not limited to genetics. Although the exact causes remain unknown, researchers believe that a variety of conditions, including environment, hormones, injury, infection, and genes, could all play a role in initiating autoimmunity. Numerous investigations demonstrate multifactorial causes of AD, including a Johns Hopkins study on patients who developed Scleroderma at the same time that their immune system was fighting cancer cells (19). Another example is psoriasis, an autoimmune skin condition that often appears within a short time after a strep throat infection (20).
In contrast with autoinflammatory disease, autoimmune conditions are quite common. Current data estimates that ADs affect at least 14 million people in the U.S. alone. There are 80-100 known autoimmune and autoimmune-related conditions, including Hashimoto’s thyroiditis, Type 1 diabetes, Sjögren’s, and celiac disease. Gender prevalence in AD is well documented. In fact, around 80% of those diagnosed are women. While ADs can affect anyone at any age, the majority tend to appear during adulthood (21).
One challenging aspect of diagnosing AD is that symptoms can vary widely—even among individuals with the same disease. Neither AD nor AIF has a standard presentation. This is just one reason why diagnosing these conditions can be a lengthy and complicated process. It also underscores the need for further scientific investigations and efforts to promote awareness.
Other Similarities
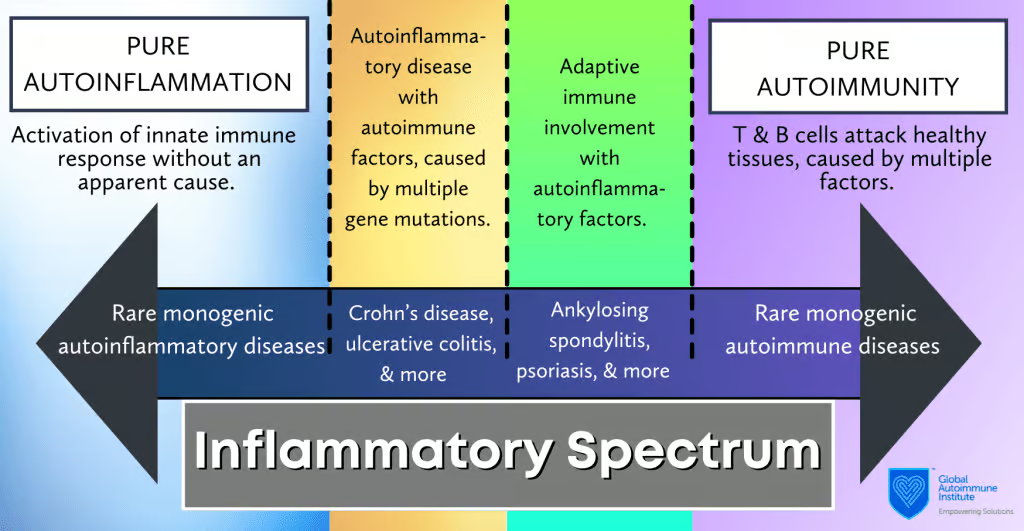
Although it is helpful to differentiate inflammatory disorders based on their involvement with innate or adaptive immunity, some conditions have combined features of autoimmune and autoinflammatory disease. As such, many researchers note that AIF and AD, rather than being two distinct groups, could actually be part of a spectrum of inflammatory disorders (22, 23). Diseases that involve both types of immunity include ankylosing spondylitis, psoriatic arthritis, Behcet’s disease, Crohn’s disease, and more (24).
Conclusion
Autoinflammatory and autoimmune conditions belong to a complex group of diseases characterized by immune system dysregulation. While scientists continue to search for answers involving the mechanisms of these diseases, it is clear that immune-related illnesses are becoming more prevalent in Western nations. Adding to the enormous importance of studying these conditions, chronic inflammation is linked to numerous other health concerns, including heart disease, cancer, stroke, and more (25). In order to improve strategies for diagnosis, treatment, and patient support, it is key that researchers continue their commitment to improving knowledge about inflammatory disorders.
Sources
- Article Sources
Warrington, R., Watson, W., Kim, H.L. et al. (2011). An introduction to immunology and immunopathology. All Asth Clin Immun.
Institute for Quality and Efficiency in Health Care. (2006). The innate and adaptive immune systems.
Molnar, C., & Gair, J. (2015). Concepts of Biology – 1st Canadian Edition. BCcampus.
Arango Duque, G. & Descoteaux, A. (2014) Macrophage cytokines: involvement in immunity and infectious diseases. Front. Immunol.
Cano, R.L.E. & Lopera, H.D.E. (2013). Introduction to T and B lymphocytes. El Rosario University Press.
Thompson, A.E. The Immune System. JAMA.
Centers for Disease Control and Prevention (2021). Antigenic Characterization.
Chaplin, D.D. Overview of the immune response. (2010). J Allergy Clin Immunol.
National Institute of Allergy and Infectious Disease (2014). Immune Tolerance.
The Walter and Eliza Hall Institute of Medical Research (2021). Autoinflammatory Diseases.
British Society for Immunology. Autoinflammation.
Cush, J.J. (2013). Autoinflammatory syndromes. Dermatol Clin.
Masters S.L., Simon A., Aksentijevich I., Kastner D.L. Horror autoinflammaticus: the molecular pathophysiology of autoinflammatory disease. (2009). Annu Rev Immunol.
De Sanctis, S., Nozzi, M., Del Torto, M. et al. (2010). Autoinflammatory syndromes: diagnosis and management. Ital J Pediatr.
Navallas, M., Inarejos Clemente, E.J., Iglesias, E. et al. (2020). Autoinflammatory diseases in childhood, part 1: monogenic syndromes. Pediatr Radiol.
Mulders-Manders, C.M., van der Hilst, J.C.H., van der Meer, J.W.M., & Simon, A. (2019). Systemic Autoinflammatory Syndromes. Clinical Immunology (Fifth Edition).
McGonagle D., McDermott M.F. (2006) A Proposed Classification of the Immunological Diseases. PLoS Med.
Caso F., Galozzi P., Costa L., et al. Autoinflammatory granulomatous diseases: from Blau syndrome and early-onset sarcoidosis to NOD2-mediated disease and Crohn’s disease. RMD Open.
Darrah, E. (2017). Systematic autoantigen analysis identifies a distinct subtype of scleroderma with coincident cancer. Johns Hopkins Rheumatology.
Autoimmune Disease: Why Is My Immune System Attacking Itself?. Johns Hopkins University.
Angum F, Khan T, Kaler J, Siddiqui L, Hussain A. (2020). The Prevalence of Autoimmune Disorders in Women: A Narrative Review. Cureus.
El-Shebiny, E.M., Zahran, E.S., Shoeib, S.A. et al. (2021). Bridging autoinflammatory and autoimmune diseases. Egypt J Intern Med.
Rosenbaum, J. Spondyloarthritis: Autoimmune or Autoinflammatory? Spondylitis Association of America.
Mauro, D., Thomas, R., Guggino, G. et al. (2021). Ankylosing spondylitis: an autoimmune or autoinflammatory disease?. Nat Rev Rheumatol.
Arakelyan A, Nersisyan L, Poghosyan D, et al. (2017). Autoimmunity and autoinflammation: A systems view on signaling pathway dysregulation profiles. PLoS One.